Working with organizations big and small throughout the nation has unique benefits, the most amazing of which has been watching trends across geographic regions, specialties, and demographics. One such trend seems to indiscriminately apply to various locations, including private practices, sprawling hospital campuses, and even rural hospital centers: it is easy to get lost in the maze of everything that must be done to create and maintain a strong revenue cycle. So many unique industry requirements, ever-changing regulations, and increasing reimbursement challenges demand attention.
Too often, we are chasing down a specific denial reason for hours or something unexpected on a remittance creates confusion that sends us down the rabbit hole of reviewing payer policy guidelines and testing the limits of our payer portal access. The only tried and true method to achieve and maintain a successful revenue cycle is through the careful creation of a strong foundation alongside ongoing attention to and focus on the entire revenue cycle.
In other words, instead of chasing fires, go back to the basics to create solid preventive strategies that minimize the likelihood of combustion within your revenue cycle. To do that we need a firm understanding of the basics. Consider this article an evergreen primer for revenue cycle management basics.
Step 1: Understanding the Revenue Cycle
The revenue cycle includes every step from the first patient call until after the payment for services has been received, posted, and analyzed. Meaning the front desk, intake team, providers, billers, coders, and reporting specialists all have a role to play in its success or failure.
Real-World Challenge
A midsized private practice in the Midwest had high turnover in its billing department for failure to meet collections goals and having exceedingly high write-offs. Further review identified that the write-offs were due to errors made at the point of check-in, which created unpayable/unresolvable claims.
Primary Issue
A failure to understand the importance of open communication and collaboration necessary for revenue cycle improvement.
Step 2: Foundation Is a Requirement
Once a facility has been set up, it is easy to forget or forgo the review of foundational items. These critical components may change and evolve but their inaccuracy at any phase can impact reimbursement. That includes correct national provider identifier setup, payer contracting, current payer participation lists, proper use of taxonomy codes, updated technologies, standard operating procedures, current fee schedules, educated staff, and compliant operations.
Real World Challenge
A small practice on the West Coast had very low reimbursement for their nurse practitioners (NPs).
Primary Issue
The practice had undergone a change in management a few months after the start of the 2 NPs, and credentialing was never completed.
Step 3: Focus on the Revenue Cycle in 4 Phases
When we break the revenue cycle down into consumable chunks, we can assess the roles that fall under each phase.
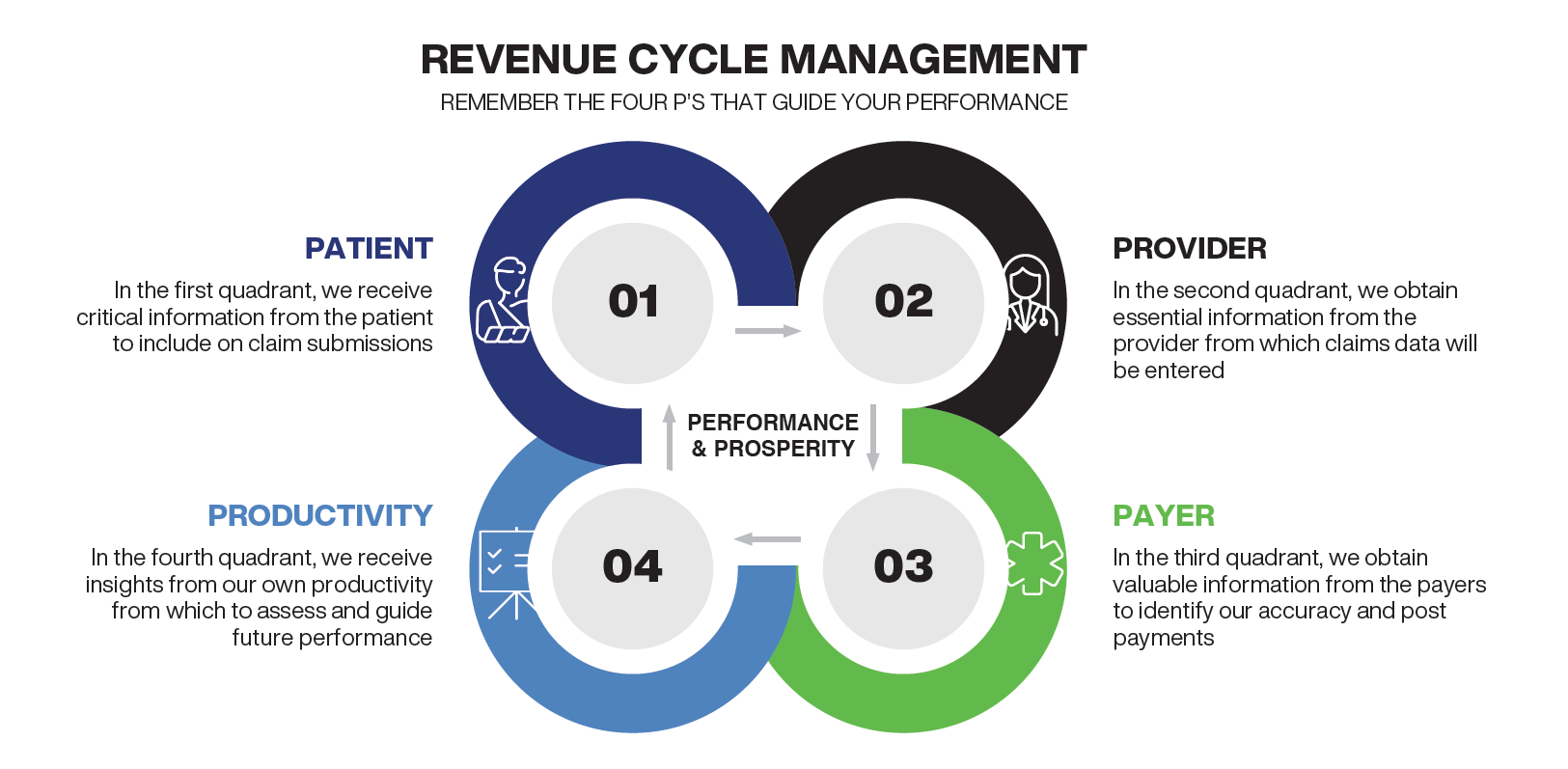
Phase 1: Information From the Patient
This section covers the initial patient intake; eligibility and benefits verification; appointment management; and intake on the actual date of service, including collection of patient payment responsibilities at the time of service.
Phase 2: Information From the Provider
This phase focuses on what happened with the patient and translating that into a chart and eventually a claim. It includes provider documentation, coding, charge entry, claims preparation, scrubbing, and submission.
Phase 3: Information From the Payer
At this point, the organization starts to assess the other half of the conversation, often called midcycle or the back half of the revenue cycle. In this phase, we include deposit management, internal controls, payment posting, receipt of payment, and aging receivables collections.
Phase 4: Information From Performance
In this phase, we evaluate our own productivity and performance. This includes using key performance indicators and other metrics to measure against appropriate industry benchmarks. Also included are quality and value-based program management and evaluation as well as overall reporting and analytics to drive overall revenue cycle strategy.
So how does an organization focus on all of these items? One phase at a time. Map the phases to the quarters in the calendar year and intentionally set strategy for each quarter.
Q1 = Phase 1
January through March—focus on improvement when collecting information from patients. Accuracy is key. Many patients will have insurance changes that need to be entered, which means this is an apt time to deploy a strategy for cleaner collection and entry of demographic and appointment data.
Create a strategy that focuses on shoring up the basic foundational components of revenue cycle management, optimizing the use of technology, and engaging your team in full cycle collaboration.
Q2 = Phase 2
April through June—focus on improvement of documentation and coding. Review CPT codes that may have changed, or schedule annual coding audits to occur during this time. Do staff members have the skill set to do the jobs to which they are assigned? Does the entire team have updated coding books?
Q3 = Phase 3
July through September—focus on the information coming in from providers. Does the entire team (front desk, billing, etc) have access to the portals they need to effectively communicate with payers? Are there any changes to electronic data interchange setup screens that need to be done during this time? Take time to review the initial proposed rulings from the Centers for Medicare & Medicaid Services that come out each year during this time.
Q4 = Phase 4
October through December—focus on your own productivity and performance. How does your organization compare to like-sized facilities in similar geographic regions? Have you performed your security risk assessment to ensure your data are safeguarded against bad actors? What payers are creating revenue cycle challenges with denial rates or velocity slowdowns? What critical areas do you want to focus on going into the new year?
There is so much happening within the revenue cycle that it is easy to miss seeing the forest for the trees. The key to long-term financial success is intentionality and prevention. Create a strategy that focuses on shoring up the basic foundational components of revenue cycle management, optimizing the use of technology, and engaging your team in full cycle collaboration. Then it’s just a matter of continuing to improve upon that strategy year over year.