As healthcare leaders, we are in a constant state of change. Many of us wear multiple hats and rely heavily on our abilities to lead in the present while keeping a watchful eye on what lies ahead. To remain successful, it is important to identify factors that can affect our organizations now and in the future. We can then use this information to refine our approach to problem solving, becoming proactive to trends, and charting new paths for our practices and team members.
The increase in telehealth and other virtual care delivery options resulting from the COVID-19 pandemic has forced us to adopt technology in ways that, as an industry, we previously avoided. However, to meet the needs of our patients, providers, and staff, we have found innovative ways to leverage this technology, which has proven to be very beneficial. For example, many patients are now able to receive care from the comfort and safety of their homes and they can make secure, virtual payments to their providers. Managers can also track remote staff productivity using dashboards and reports.
It is important to remember, however, there can be minefields within an evolving landscape. We are facing cybersecurity attacks, decreases in reimbursement, new regulations, coding updates, and increasing demands from stakeholders, among other challenges. As healthcare leaders, I believe we have the unique opportunity in the upcoming year to refine our leadership posture to set a new tone for our organizations in several key areas.
Workforce Retention
In many ways, the challenging events that transpired in 2020 and 2021 brought out the best in us. We were able to “pull back the curtain” on many of our professional relationships and see our team members for the unique individuals that they are. These members often looked to us to calm their fears, which we accomplished through effective communication, maintaining structure, and careful mentoring.
Many of us have adopted a hybrid approach to performing our jobs (eg, dividing our time between working in the office and from home). As a result, it is not uncommon for our children or pets to occasionally join us during Zoom meetings, which I believe has actually made us more candid with our colleagues and helped to build greater trust and honesty. I think we need to build on these positive experiences to foster a culture that encourages employees to stay with our organizations.
Leadership Posture
The need to refine our leadership posture is incumbent on us as workforce expectations have shifted, leading to national staffing shortages. I think it is important for us to ask ourselves, as employers, whether we have missed the mark somewhere, making it difficult to retain good talent. My suggestion is that we use the current shortage as a catalyst to initiate innovative strategies that prioritize positive experiences for all our staff members.
Call to Action
- Who are the workforce members affected by employment instability?
- What are the needs of your workforce members that have not been met? What can be done to meet these needs?
- When will organizational culture evolve to align with employment and retention trends?
- Where do you start? With yourself? With local or national trends?
- Why are workforce needs changing?
- How successful do your workforce members feel with the resources they are given to do their jobs?
Managing Stakeholders’ Expectations
As leaders in healthcare, it is imperative that we consider the unique perspective of each stakeholder, taking into account his or her role in the continuum of care. We also need to analyze stakeholders’ needs as past and future trends impact our capabilities to succeed and improve in the delivery of the outcomes they expect.
Leadership Posture
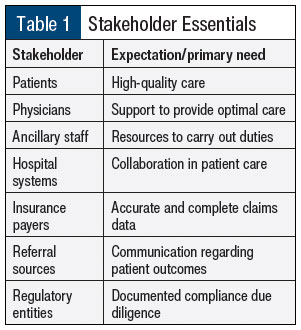
There is a quote by Kate Zabriskie that says, “The customer’s perception is your reality.” Stakeholders are our customers, and our risk for failure is dependent on their perceptions. We can minimize this risk by improving their experiences. Therefore, our leadership posture should include becoming experts at understanding and applying each stakeholder’s unique needs while simultaneously setting boundaries and realistic expectations (Table 1).
Call to Action
- Who are the stakeholders you interact with and what are your mutual goals?
- What resources are needed to meet your stakeholders’ expectations?
- When do you need to look back to see if you’ve accomplished your set goals?
- Where do your stakeholders’ need you to meet them (eg, their level, mutual level, lower level)?
- Why are your stakeholders’ expectations fluctuating?
- How can you fulfill your stakeholders’ expectations and primary needs?
PROBLEM-SOLVING AND DECISION-MAKING
The majority of a healthcare leader’s time is spent solving problems and making decisions. We are called upon for a host of resolutions, including safety concerns, electronic medical record troubleshooting, staff workflows, and complaints. Our timeliness and approach when making decisions sets the tone for the success of our organizations. Making the effort to dissect problems improves our capacity for thoughtful and effective decision-making.
Leadership Posture
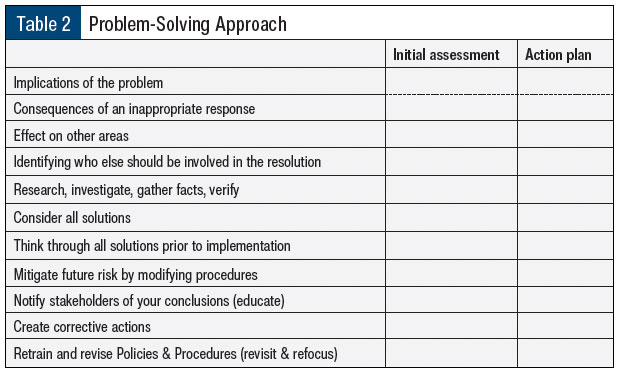
We must become masters at staying in the moment as well as thinking strategically. When inundated with daily operational needs, it is important to not lose sight of vulnerabilities that may develop or linger. We need to create opportunities that allow for root-cause correction that minimizes problems while still being decisive when resolving these problems (Table 2).
Call to Action
- Should you categorize the problem to assign appropriate team members in resolution?
- Have key aspects of the problem been documented?
- Is there anything delaying your response to the problem?
- Are there standards already in place that provide guidance for addressing the problem?
- Will the problem result in legal or financial consequences?
- Where do you turn for resources to assist with problem-solving?
Conclusion
Although 2022 will no doubt present healthcare leaders with more challenges, we can still make significant strides to overcome these obstacles by remaining proactive and considering the suggestions and strategies outlined in this article for retaining members of our workforce, meeting the needs of our stakeholders, and enhancing our problem-solving and decision-making skills. I believe the result can be a more successful and smoother running organization. This will translate to improved care for our patients, which is the ultimate goal.